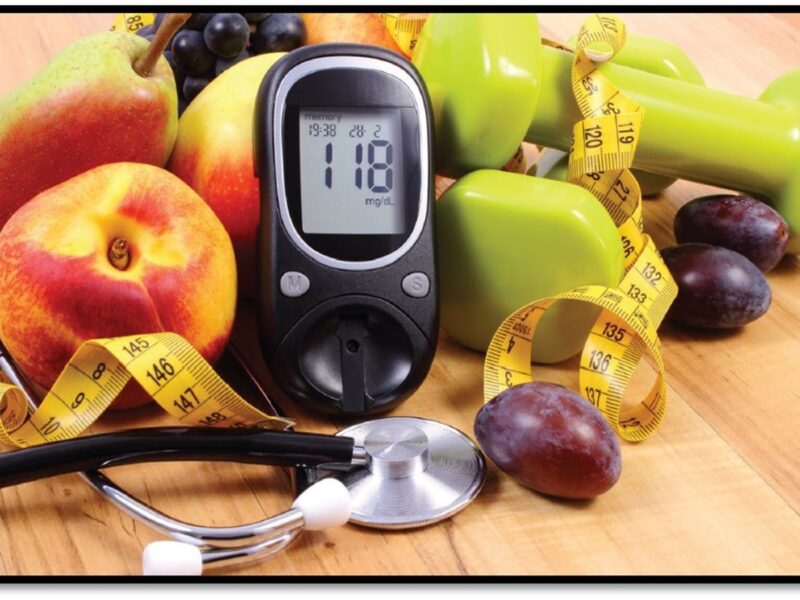
What Is Diabetes?
Diabetes is a chronic (long-lasting) health condition that affects how your body turns food into energy.
Your body breaks down most of the food you eat into sugar (glucose) and releases it into your bloodstream. When your blood sugar goes up, it signals your pancreas to release insulin. Insulin acts like a key to let the blood sugar into your body’s cells for use as energy.
With diabetes, your body doesn’t make enough insulin or can’t use it as well as it should. When there isn’t enough insulin or cells stop responding to insulin, too much blood sugar stays in your bloodstream.
Types of Diabetes
There are three main types of diabetes: type 1, type 2, and gestational diabetes (diabetes while pregnant).
Type 1 Diabetes
Type 1 diabetes is thought to be caused by an autoimmune reaction (the body attacks itself by mistake). This reaction stops your body from making insulin. Approximately 5-10% of the people who have diabetes have type 1. Symptoms of type 1 diabetes often develop quickly. It’s usually diagnosed in children, teens, and young adults. If you have type 1 diabetes, you’ll need to take insulin every day to survive. Currently, no one knows how to prevent type 1 diabetes.
Type 2 Diabetes
With type 2 diabetes, your body doesn’t use insulin well and can’t keep blood sugar at normal levels. About 90-95% of people with diabetes have type 2. It develops over many years and is usually diagnosed in adults (but more and more in children, teens, and young adults). You may not notice any symptoms, so it’s important to get your blood sugar tested if you’re at risk.
Gestational Diabetes
Gestational diabetes develops in pregnant women who have never had diabetes. If you have gestational diabetes, your baby could be at higher risk for health problems. Gestational diabetes usually goes away after your baby is born. However, it increases your risk for type 2 diabetes later in life. Your baby is more likely to have obesity as a child or teen and develop type 2 diabetes later in life.

Getting Rid Of Diabetes
Diabetes can be managed by incorporating these five things:
1. Eat A Healthy Diet
Choose to eat more whole fruits and vegetables, more whole grains and lean proteins. Get your fats from healthy sources like avocados, nuts and olive oil. Get more high-quality proteins from eggs, beans and unsweetened yogurt. Your body needs fats, carbs and proteins to function, so make sure you choose the healthiest forms! Avoid refined carbohydrates and hidden sugars. Eat whole fruits rather than drinking juice. Check food labels for hidden sugars in the ingredients list.
2. Lose weight
Losing just five to 10 percent of your body weight can help control your blood sugar, reduce your cholesterol level and lower your blood pressure. This will help reduce the risk of developing complications like heart disease and will keep you healthy.
3. Exercise
Exercising 30 minutes a day can reduce blood sugar levels, decrease insulin resistance and help regulate your blood pressure and cholesterol levels. If you can find 60 minutes per day to exercise, it can help you lose weight.

4. Get Enough Quality Sleep
Getting less than six hours of quality sleep every night can disrupt the balance of insulin and blood sugar. If you are not getting good, restful sleep, try avoiding alcohol, caffeine and spicy foods at night. You could also try lowering the temperature of your bedroom at night. Make your bedroom as dark and quiet as possible. Lastly, establish a sleep routine by going to bed and rising at the same time every day.
5. Use Your Medicine
Insulin and diabetes pills and shots are the kinds of medicines used to lower blood sugar.
Everyone with insulin-dependent diabetes (or type 1 diabetes) needs insulin, and many people with type 2 diabetes also need it.
Insulin can’t be taken as a pill. You will have to give yourself shots every day. Some people give themselves one a day. Some people give themselves two or more a day.
If your body makes insulin but it doesn’t lower your blood sugar, you may have to take diabetes pills or some other injectable. These only work in people who have some insulin of their own. Some are taken once a day, and others are taken more often. Ask your doctor when you should take yours.